Medicare Advantage Rates Are Tightening. Post-Acute Strategy Matters More Than Ever
The recently released Medicare Advantage (MA) rate notice reinforces a reality health plans already feel every day: profit margins are under increasing pressure, and they must better manage the health of their members to survive.
Overall, the Centers for Medicare and Medicaid Services (CMS) proposed a near-flat (0.1%) update in MA payment rates in 2027, even as underlying medical costs continue to rise. At the same time, CMS data shows one area growing faster than every other category in Medicare: post-acute care — particularly home health.
Post-acute spending is driving a disproportionate share of growth in Medicare spending. Home health spending is projected to increase by more than 10%—roughly 2.5x the growth rate of inpatient care. Skilled Nursing Facility (SNF) spending is projected to grow by more than 6%, about two percentage points faster than hospital care. Because MA benchmarks are based on traditional Medicare spending, growth in post-acute Fee-For-Service (FFS) costs directly flows into plan bids, even when rates themselves remain constrained.
As home health utilization grows, home health care access is a struggle for Medicare Advantage enrollees. Workforce shortages, reimbursement pressure, and increasing administrative friction mean agencies are more selective about the patients they accept. In many markets, plans are seeing longer placement times, narrower networks, and rising provider abrasion.
Together, those trends underscore how quickly utilization and dollars are shifting downstream — even as inpatient growth remains comparatively modest — and access challenges are emerging at the same pace.
With more scrutiny to risk adjustment, plans can’t rely on rate tightening or blunt utilization controls to generate savings. Instead, CMS appears to be reinforcing a shift toward care management and total cost control, particularly in high-growth areas like post-acute care. That combination creates a clear signal for Medicare Advantage leaders. Health plans must actively manage post-acute spending or continue to see margins and outcomes to erode.
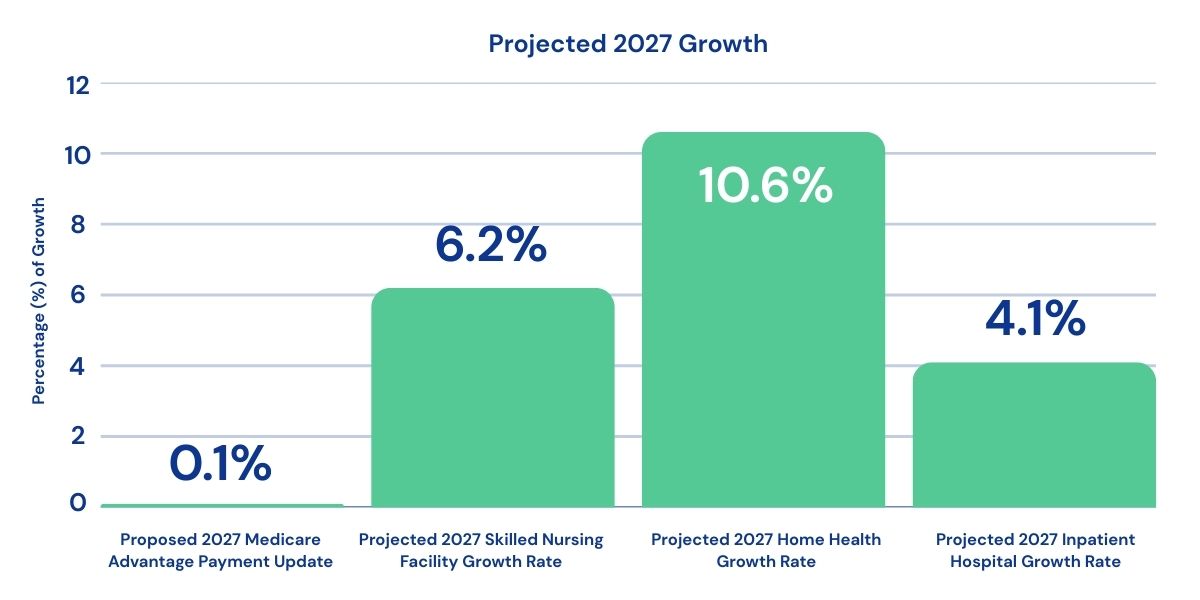
Source: CMS Office of the Actuary, Advance Notice of Methodological Changes for CY 2027
Home health is growing, and it’s not slowing down
According to CMS, growth in home health spending is being driven by both utilization and unit costs, reflecting broader trends of an aging population, pressure to discharge patients sooner, and strong patient preference for recovering at home.
For years, post-acute care has been managed largely through utilization controls like eligibility checks, visit caps, and administrative hurdles designed to limit volume. But those approaches were built for a different era.
Today’s challenge is delivering better care:
- Are members getting into home health quickly after discharge?
- Are referrals going to high-quality providers who can prevent avoidable readmissions?
- Are incentives aligned so agencies are rewarded for outcomes, not volume?
- Is care being coordinated across settings, or fragmented across vendors?
When post-acute care is treated as a transactional benefit rather than a managed episode, plans lose the trust of patients, providers disengage, and avoidable costs show up later, often as readmissions, ED visits, or extended facility stays.
A shift toward coordinated, value-based post-acute care
Instead, MA plans need a different solution: tighter integration, better care management, and accountability for total cost of care.
This is where tango’s model aligns squarely with the moment. By managing post-acute referrals at the point of discharge, tango reduces placement delays and increases access to high-performing providers.
Rather than relying on utilization management alone, tango actively manages post-acute episodes end-to-end. That means:
- Improving access by reducing placement delays and directing referrals to high-performing providers
- Aligning incentives through value-based, episodic reimbursement rather than volume-driven payments
- Reducing friction for plans and providers by integrating referral management, utilization oversight, and claims into a single delegated model
- Driving better outcomes through real-time clinical oversight and accountability across the episode of care
For plans, the result is a more sustainable way to manage one of the fastest-growing areas of spend without sacrificing quality or member experience. For providers, it creates predictability, partnership, and incentives that reward good care.
The takeaway for MA leaders
Margin protection won’t come from across-the-board cuts or tighter gates alone. It will come from smarter care delivery, especially in high-growth areas like post-acute care.
Plans that invest now in coordinated, value-based post-acute strategies will be better positioned to absorb cost pressure, improve outcomes, and compete on member experience. Those that don’t may find that unmanaged growth quietly undermines both financial performance and quality metrics.
Home health isn’t just a cost center. Managed well, it’s a lever for better care and a competitive advantage.
Turning Post-Acute Care into a Competitive Advantage
tango partners with Medicare Advantage plans to transform post-acute care from a cost center into a performance driver. Our delegated model improves placement speed, aligns providers around outcomes, and delivers predictable savings, all while protecting member access.
If you’re rethinking your post-acute strategy in light of the 2027 rate notice, we’d welcome a conversation.
